Functional Gastrointestinal Disorders and Behavioural Challenges in Children with Developmental Delays
Functional Gastrointestinal Disorders (FGIDs) are very common in children with developmental delays. Although medical tests often show no visible disease, these conditions cause genuine discomfort. The connection between functional gastrointestinal disorders and behavioural challenges in children lies in the gut–brain axis — a powerful communication system linking digestion, emotions, and neurological regulation. For children with autism spectrum disorder (ASD), ADHD, or sensory processing differences, this gut–brain interaction can amplify both physical pain and emotional responses. Understanding how FGIDs affect behaviour helps parents respond with empathy rather than assuming defiance.
Understanding FGIDs and the Gut–Brain Axis Connection
FGIDs include conditions such as functional abdominal pain, functional constipation, and paediatric irritable bowel syndrome. In these disorders, the structure of the digestive tract appears normal, but its function is altered. The nerves in the gut become hypersensitive, and communication with the brain becomes exaggerated. In children with FGIDs, even mild digestive processes may feel intense. The gut–brain axis in paediatric functional disorders becomes overactive, meaning signals between the digestive system and the brain are amplified. As a result, normal sensations may be interpreted as pain or discomfort.
In this heightened state, the following patterns commonly occur:
- Mild gas feels painful or overwhelming
- Normal digestion creates discomfort
- Emotional stress increases gut symptoms
- Gut pain feeds anxiety back to the brain
- The stress–pain cycle becomes chronic
This two-way feedback loop between digestive
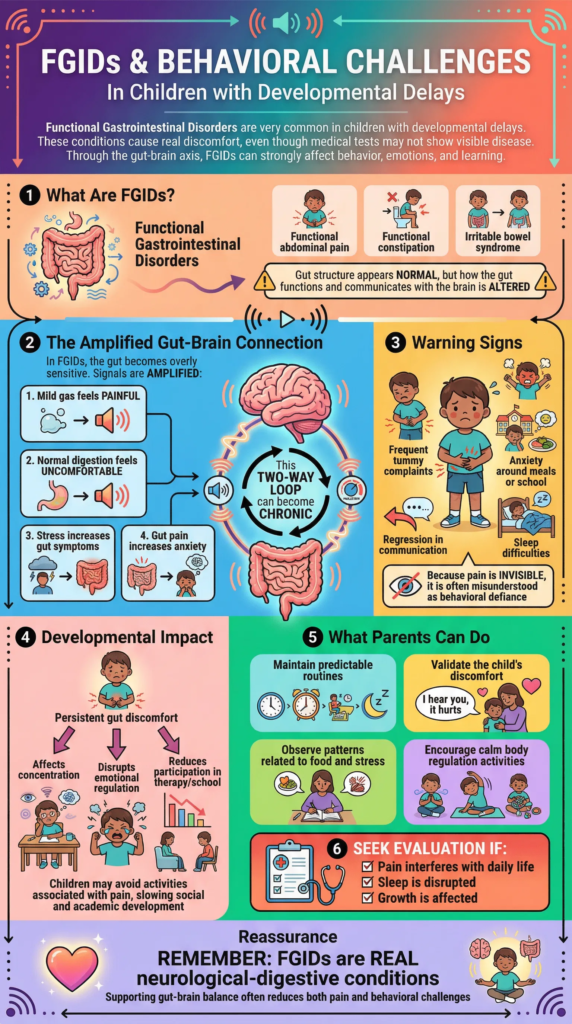
sensitivity and emotional regulation challenges can significantly affect daily functioning. . A child who appears moody or reactive may actually be coping with invisible abdominal pain.
Your Attractive Heading
Because FGIDs do not show up clearly on routine medical tests, behavioural symptoms are often the first clues. Recognizing early signs of gut-related behavioural challenges in children can prevent misunderstanding and delayed support.
Parents may notice:
- Frequent tummy complaints without infection
- Behavioural outbursts without a clear external trigger
- Anxiety around meals, school, or transitions
- Sleep disturbances or difficulty settling at night
- Regression in communication or daily living skills
When pain is invisible, it is frequently mistaken for attention-seeking or oppositional behaviour. However, persistent abdominal discomfort can reduce a child’s tolerance for frustration and increase emotional reactivity. The impact of chronic gut discomfort on learning and development is significant. Children struggling with abdominal pain may find it difficult to concentrate in school or participate in therapy sessions. Avoidance behaviours can develop if a child begins associating certain activities with discomfort.
Developmental and Emotional Impact of FGIDs
Ongoing digestive sensitivity can interfere with attention span, memory retention, and social engagement. When the nervous system is focused on managing internal discomfort, fewer resources remain for processing new information or navigating social situations. Over time, chronic stress linked to FGIDs may lower self-confidence. A child who repeatedly feels unwell may withdraw from peer activities or structured learning environments. Addressing gut–brain balance early helps protect both emotional wellbeing and academic progress.
Supportive Strategies for Managing FGIDs at Home
Consistent daily routines and emotional validation play a crucial role in managing paediatric FGIDs. Supporting both digestive function and stress regulation can reduce symptom intensity.
Parents can:
- Maintain predictable daily routines
- Validate the child’s discomfort without dismissal
- Observe patterns related to food intake and stress triggers
- Encourage calm body regulation activities such as deep breathing
- Promote regular sleep and balanced hydration
These supportive habits help stabilize the gut–brain communication system and reduce flare-ups.
When to Seek Medical Evaluation
Medical evaluation is important if abdominal pain interferes with daily life, sleep, appetite, or growth. A paediatrician or paediatric gastroenterologist can assess for FGIDs and rule out other gastrointestinal conditions. Early intervention improves long-term outcomes.
Reassurance for Parents
Functional Gastrointestinal Disorders are real neurological–digestive conditions, not behavioural manipulation. By supporting gut health and emotional regulation together, families often see meaningful reductions in pain and behavioural challenges, allowing children to participate more confidently in learning and social experiences.