Abdominal Pain and Behavioural Changes in Children: Understanding the Gut–Brain Connection
Abdominal pain in children is common, but in children with developmental delays, it is often misunderstood or overlooked. When a child struggles to express discomfort verbally, tummy pain may appear as sudden mood shifts or challenging behaviours. Understanding the gut–brain connection in children can help parents respond with empathy instead of frustration. The relationship between abdominal pain and behavioural changes in children is strongly linked to the gut–brain axis. This two-way communication system connects the digestive system and the brain, meaning physical discomfort in the belly can directly influence emotions, attention, and behaviour.
What Is Abdominal Pain in Children?
Abdominal pain refers to discomfort, cramping, bloating, burning, or pressure anywhere in the stomach area. While older children may say, “My stomach hurts,” younger children or those with communication challenges may not be able to describe what they feel. Instead of clearly reporting pain, children may show behavioural signs of stomach pain such as irritability, clinginess, withdrawal, or sudden emotional outbursts. For children with sensory processing difficulties, even mild gut discomfort can feel overwhelming. Recognizing hidden abdominal pain symptoms in children is especially important for parents of children with autism, ADHD, or developmental delays.
How the Gut–Brain Axis Affects Behaviour
The gut and brain are connected through nerves, hormones, and immune signals. One of the key pathways is the vagus nerve, which carries signals from the digestive tract directly to the brain. When pain receptors in the gut are activated, the brain responds by increasing stress and alertness.
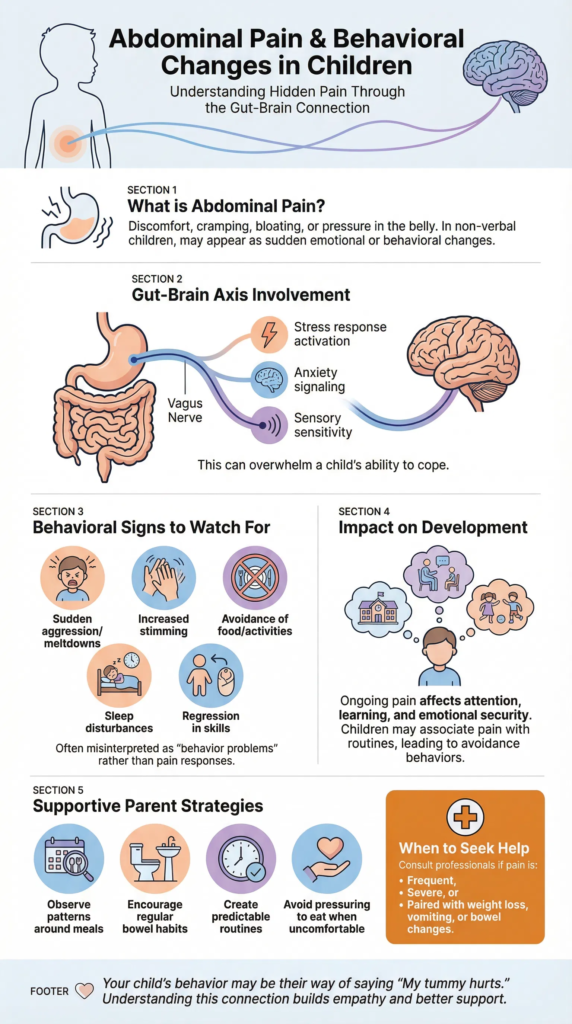
Chronic digestive discomfort in children can lead to:
- Increased stress response activation
- Heightened anxiety signalling
- Greater sensory sensitivity
- Difficulty regulating emotions
- Reduced tolerance for routine changes
When the nervous system is already overloaded, even small triggers can lead to meltdowns or shutdowns. This explains why stomach pain and emotional dysregulation in children are often closely linked.
Behavioural Signs of Hidden Tummy Pain
Children who cannot explain abdominal discomfort may communicate through behaviour. These responses are not intentional misbehaviour but attempts to cope with internal distress.
Parents may observe:
- Sudden aggression or intense meltdowns
- Increased stimming or repetitive behaviours
- Refusal to eat or avoidance of certain foods
- Sleep disturbances or frequent night waking
- Regression in communication or self-care skills
These behaviours are frequently misinterpreted as discipline problems rather than physical pain signals. Understanding behavioural changes caused by abdominal pain allows caregivers to respond with support instead of punishment.
Impact on Learning and Development
Ongoing abdominal pain can significantly affect a child’s development. Chronic discomfort drains mental energy, making it harder to focus, process information, and participate in therapy sessions. Over time, children may associate specific environments—such as school or therapy—with discomfort, leading to avoidance behaviours. Abdominal pain and attention difficulties in children often go hand in hand. Emotional security may also be affected, especially if the child feels misunderstood or repeatedly corrected for behaviour that is pain-driven.
Supportive Strategies for Parents
Parents play a key role in identifying patterns and reducing discomfort. Observing when pain appears—such as after certain foods, during constipation, or around stressful events—can provide helpful clues.
Helpful strategies include:
- Tracking meal times and behaviour patterns
- Encouraging regular bowel habits and hydration
- Maintaining predictable daily routines
- Reducing pressure around eating when discomfort is present
- Creating a calm environment during flare-ups
These approaches support both digestive health and emotional regulation.
When to Seek Professional Help
Consult a healthcare professional if abdominal pain is frequent, severe, or accompanied by symptoms such as weight loss, vomiting, persistent constipation, diarrhea, or blood in stool. Early medical evaluation can rule out underlying gastrointestinal issues and provide targeted treatment.
A Reassuring Reminder for Parents
Sometimes behaviour is a child’s only way of saying, “My tummy hurts.” By recognizing the connection between abdominal pain and behavioural changes in children, parents can respond with compassion and proactive support. Understanding the gut–brain relationship builds empathy, strengthens trust, and helps children feel safe and understood.